Carpal tunnel syndrome
Carpal tunnel syndrome (CTS) is a medical condition due to compression of the median nerve as it travels through the wrist at the carpal tunnel.[1] The main symptoms are pain, numbness and tingling in the thumb, index finger, middle finger and the thumb side of the ring finger.[1] Symptoms typically start gradually and during the night.[2] Pain may extend up the arm.[2] Weak grip strength may occur, and after a long period of time the muscles at the base of the thumb may waste away.[2] In more than half of cases, both hands are affected.[1]
| Carpal tunnel syndrome | |
|---|---|
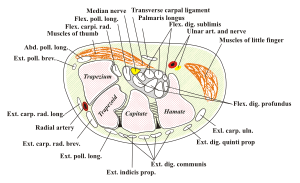 | |
| Transverse section at the wrist. The median nerve is colored yellow. The carpal tunnel consists of the bones and transverse carpal ligament. | |
| Specialty | Orthopedic surgery, plastic surgery |
| Symptoms | Pain, numbness, tingling in the thumb, index, middle finger, and half of ring finger, weak grip[1][2] |
| Causes | Compression of the median nerve at the carpal tunnel[1] |
| Risk factors | Genetics, obesity, repetitive wrist work, pregnancy, rheumatoid arthritis[3][4][5] |
| Diagnostic method | Based on symptoms, specific physical tests, electrodiagnostic tests[2] |
| Prevention | Physical activity[3] |
| Treatment | Wrist splint, corticosteroid injections, surgery[3] |
| Frequency | 5–10%[6][7] |
Risk factors include obesity, repetitive wrist work, pregnancy, genetics, and rheumatoid arthritis.[3][4][5] There is tentative evidence that hypothyroidism increases the risk.[8] Diabetes mellitus is weakly associated with CTS.[3][7] The use of birth control pills does not affect the risk.[3] Types of work that are associated include computer work, work with vibrating tools and work that requires a strong grip.[3] Diagnosis is suspected based on signs, symptoms and specific physical tests and may be confirmed with electrodiagnostic tests.[2] If muscle wasting at the base of the thumb is present, the diagnosis is likely.[3]
Being physically active can decrease the risk of developing CTS.[3] Symptoms can be improved by wearing a wrist splint or with corticosteroid injections.[3] Taking NSAIDs or gabapentin does not appear to be useful.[3] Surgery to cut the transverse carpal ligament is effective with better results at a year compared to non-surgical options.[3] Further splinting after surgery is not needed.[3] Evidence does not support magnet therapy.[3]
About 5% of people in the United States have carpal tunnel syndrome.[6] It usually begins in adulthood, and women are more commonly affected than men.[2] Up to 33% of people may improve without specific treatment over approximately a year.[1] Carpal tunnel syndrome was first fully described after World War II.[9]
Signs and symptoms
People with CTS experience numbness, tingling, or burning sensations in the thumb and fingers, in particular the index and middle fingers and radial half of the ring finger, because these receive their sensory and motor function (muscle control) from the median nerve. Ache and discomfort can possibly be felt more proximally in the forearm or even the upper arm.[10] Less-specific symptoms may include pain in the wrists or hands, loss of grip strength,[11] and loss of manual dexterity.[12]
Some suggest that median nerve symptoms can arise from compression at the level of the thoracic outlet or the area where the median nerve passes between the two heads of the pronator teres in the forearm,[13] although this is debated.
Numbness and paresthesias in the median nerve distribution are the hallmark neuropathic symptoms (NS) of carpal tunnel entrapment syndrome.[7] Weakness and atrophy of the thumb muscles may occur if the condition remains untreated, because the muscles are not receiving sufficient nerve stimulation.[7] Discomfort is usually worse at night and in the morning.
Causes
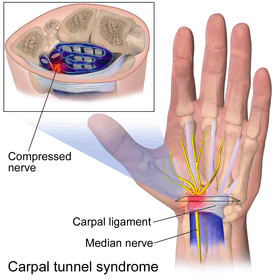
Most cases of CTS are of unknown cause.[14] Risk factors include obesity, repetitive wrist work, pregnancy, genetics, and rheumatoid arthritis.[3][4][5] There is tentative evidence that hypothyroidism increases the risk.[8] Diabetes mellitus is weakly associated with CTS.[3][7] The use of birth control pills does not affect the risk.[3] Types of work that are associated include computer work, work with vibrating tools and work that requires a strong grip.[3]
Trauma may also place a role,[15] as may genetics.[16] Carpal tunnel is a feature of a form of Charcot-Marie-Tooth syndrome type 1 called hereditary neuropathy with susceptibility to pressure palsies.
Other causes of this condition include intrinsic factors that exert pressure within the tunnel, and extrinsic factors (pressure exerted from outside the tunnel), which include benign tumors such as lipomas, ganglion, and vascular malformation.[17] Severe carpal tunnel syndrome often is a symptom of transthyretin amyloidosis-associated polyneuropathy and prior carpal tunnel syndrome surgery is very common in individuals who later present with transthyretin amyloid-associated cardiomyopathy, suggesting that transthyretin amyloid deposition may cause carpal tunnel syndrome in these people.[18]
The median nerve can usually move up to 9.6 mm to allow the wrist to flex, and to a lesser extent during extension.[19] Long-term compression of the median nerve can inhibit nerve gliding, which may lead to injury and scarring. When scarring occurs, the nerve will adhere to the tissue around it and become locked into a fixed position, so that less movement is apparent.[20]
Normal pressure of the carpal tunnel has been defined as a range of 2–10 mm, and wrist flexion increases this pressure 8-fold, while extension increases it 10-fold.[19] Repetitive flexion and extension in the wrist significantly increase the fluid pressure in the tunnel through thickening of the synovial tissue that lines the tendons within the carpal tunnel.[21]
Genetics
Genetic factors are believed to be the most important determinants of who develops carpal tunnel syndrome.[5] A genome-wide association study (GWAS) of carpal tunnel syndrome identified 16 genomic loci significantly associated with the disease, including several loci previously known to be associated with human height.[22]
Work related
The international debate regarding the relationship between CTS and repetitive motion in work is ongoing. The Occupational Safety and Health Administration (OSHA) has adopted rules and regulations regarding cumulative trauma disorders. Occupational risk factors of repetitive tasks, force, posture, and vibration have been cited. The relationship between work and CTS is controversial; in many locations, workers diagnosed with carpal tunnel syndrome are entitled to time off and compensation.[23][24]
Some speculate that carpal tunnel syndrome is provoked by repetitive movement and manipulating activities and that the exposure can be cumulative. It has also been stated that symptoms are commonly exacerbated by forceful and repetitive use of the hand and wrists in industrial occupations,[25] but it is unclear as to whether this refers to pain (which may not be due to carpal tunnel syndrome) or the more typical numbness symptoms.[26]
A review of available scientific data by the National Institute for Occupational Safety and Health (NIOSH) indicated that job tasks that involve highly repetitive manual acts or specific wrist postures were associated with incidents of CTS, but causation was not established, and the distinction from work-related arm pains that are not carpal tunnel syndrome was not clear. It has been proposed that repetitive use of the arm can affect the biomechanics of the upper limb or cause damage to tissues. It has also been proposed that postural and spinal assessment along with ergonomic assessments should be included in the overall determination of the condition. Addressing these factors has been found to improve comfort in some studies.[27] A 2010 survey by NIOSH showed that 2/3 of the 5 million carpal tunnel cases in the US that year were related to work.[28] Women have more work-related carpal tunnel syndrome than men.[29]
Speculation that CTS is work-related is based on claims such as CTS being found mostly in the working adult population, though evidence is lacking for this. For instance, in one recent representative series of a consecutive experience, most patients were older and not working.[30] Based on the claimed increased incidence in the workplace, arm use is implicated, but the weight of evidence suggests that this is an inherent, genetic, slowly but inevitably progressive idiopathic peripheral mononeuropathy.[31]
Associated conditions
A variety of patient factors can lead to CTS, including heredity, size of the carpal tunnel, associated local and systematic diseases, and certain habits.[32] Non-traumatic causes generally happen over a period of time, and are not triggered by one certain event. Many of these factors are manifestations of physiologic aging.[33]
Examples include:
- Rheumatoid arthritis and other diseases that cause inflammation of the flexor tendons.
- With hypothyroidism, generalized myxedema causes deposition of mucopolysaccharides within both the perineurium of the median nerve, as well as the tendons passing through the carpal tunnel.
- During pregnancy, women commonly experience CTS due to hormonal changes (high progesterone levels) and water retention, which swells the synovium
- Previous injuries including fractures of the wrist.
- Medical disorders that lead to fluid retention or are associated with inflammation such as: inflammatory arthritis, Colles' fracture, amyloidosis, hypothyroidism, diabetes mellitus, acromegaly, and use of corticosteroids and estrogens.
- Carpal tunnel syndrome is also associated with repetitive activities of the hand and wrist, in particular with a combination of forceful and repetitive activities[15]
- Acromegaly causes excessive secretion of growth hormones. This causes the soft tissues and bones around the carpel tunnel to grow and compress the median nerve.[34]
- Tumors (usually benign), such as a ganglion or a lipoma, can protrude into the carpal tunnel, reducing the amount of space. This is exceedingly rare (less than 1%).
- Obesity also increases the risk of CTS: individuals classified as obese (BMI > 29) are 2.5 times more likely than slender individuals (BMI < 20) to be diagnosed with CTS.[35]
- Double-crush syndrome is a debated hypothesis that compression or irritation of nerve branches contributing to the median nerve in the neck, or anywhere above the wrist, increases sensitivity of the nerve to compression in the wrist. There is little evidence, however, that this syndrome really exists.[36]
- Heterozygous mutations in the gene SH3TC2, associated with Charcot-Marie-Tooth, confer susceptibility to neuropathy, including the carpal tunnel syndrome.[37]
Pathophysiology
The carpal tunnel is an anatomical compartment located at the base of the palm. Nine flexor tendons and the median nerve pass through the carpal tunnel that is surrounded on three sides by the carpal bones that form an arch. The median nerve provides feeling or sensation to the thumb, index finger, long finger, and half of the ring finger. At the level of the wrist, the median nerve supplies the muscles at the base of the thumb that allow it to abduct, move away from the other four fingers, as well as move out of the plane of the palm. The carpal tunnel is located at the middle third of the base of the palm, bounded by the bony prominence of the scaphoid tubercle and trapezium at the base of the thumb, and the hamate hook that can be palpated along the axis of the ring finger. From the anatomical position, the carpal tunnel is bordered on the anterior surface by the transverse carpal ligament, also known as the flexor retinaculum. The flexor retinaculum is a strong, fibrous band that attaches to the pisiform and the hamulus of the hamate. The proximal boundary is the distal wrist skin crease, and the distal boundary is approximated by a line known as Kaplan's cardinal line.[38] This line uses surface landmarks, and is drawn between the apex of the skin fold between the thumb and index finger to the palpated hamate hook.[39] The median nerve can be compressed by a decrease in the size of the canal, an increase in the size of the contents (such as the swelling of lubrication tissue around the flexor tendons), or both.[40] Since the carpal tunnel is bordered by carpal bones on one side and a ligament on the other, when the pressure builds up inside the tunnel, there is nowhere for it to escape and thus it ends up pressing up against and damaging the median nerve. Simply flexing the wrist to 90 degrees will decrease the size of the canal.
Compression of the median nerve as it runs deep to the transverse carpal ligament (TCL) causes atrophy of the thenar eminence, weakness of the flexor pollicis brevis, opponens pollicis, abductor pollicis brevis, as well as sensory loss in the digits supplied by the median nerve. The superficial sensory branch of the median nerve, which provides sensation to the base of the palm, branches proximal to the TCL and travels superficial to it. Thus, this branch spared in carpal tunnel syndrome, and there is no loss of palmar sensation.[41]
Diagnosis
There is no consensus reference standard for the diagnosis of carpal tunnel syndrome. A combination of described symptoms, clinical findings, and electrophysiological testing may be used. Correct diagnosis involves identifying if symptoms matches the distribution pattern of the median nerve (which does not normally include the 5th digit).
CTS work up is the most common referral to the electrodiagnostic lab. Historically, diagnosis has been made with the combination of a thorough history and physical examination in conjunction with the use of electrodiagnostic (EDX) testing for confirmation. Additionally, evolving technology has included the use of ultrasonography in the diagnosis of CTS. However, it is well established that physical exam provocative maneuvers lack both sensitivity and specificity. Furthermore, EDX cannot fully exclude the diagnosis of CTS due to the lack of sensitivity. A Joint report published by the American Association of Neuromuscular and Electrodiagostic Medicine (AANEM), the American Academy of Physical Medicine and Rehabilitation (AAPM&R) and the American Academy of Neurology defines practice parameters, standards and guidelines for EDX studies of CTS based on an extensive critical literature review. This joint review concluded median and sensory nerve conduction studies are valid and reproducible in a clinical laboratory setting and a clinical diagnosis of CTS can be made with a sensitivity greater than 85% and specificity greater than 95%. Given the key role of electrodiagnostic testing in the diagnosis of CTS, The American Association of Neuromuscular & Electrodiagnostic Medicine has issued evidence-based practice guidelines, both for the diagnosis of carpal tunnel syndrome.
Numbness in the distribution of the median nerve, nocturnal symptoms, thenar muscle weakness/atrophy, positive Tinel's sign at the carpal tunnel, and abnormal sensory testing such as two-point discrimination have been standardized as clinical diagnostic criteria by consensus panels of experts.[42][43] Pain may also be a presenting symptom, although less common than sensory disturbances.
Electrodiagnostic testing (electromyography and nerve conduction velocity) can objectively verify the median nerve dysfunction. Normal nerve conduction studies, however, do not exclude the diagnosis of CTS. Clinical assessment by history taking and physical examination can support a diagnosis of CTS. If clinical suspicion of CTS is high, treatment should be initiated despite normal electrodiagnostic testing.
Physical exam
Although widely used, the presence of a positive Phalen test, Tinel sign, Flick sign, or upper limb nerve test alone is not sufficient for diagnosis.[3]
- Phalen's maneuver is performed by flexing the wrist gently as far as possible, then holding this position and awaiting symptoms.[44] A positive test is one that results in numbness in the median nerve distribution when holding the wrist in acute flexion position within sixty seconds. The quicker the numbness starts, the more advanced the condition. Phalen's sign is defined as pain or paresthesias in the median-innervated fingers with one minute of wrist flexion. Only this test has been shown to correlate with CTS severity when studied prospectively.[32] The test characteristics of Phalen's maneuver have varied across studies ranging from 42–85% sensitivity and 54–98% specificity.[7]
- Tinel's sign is a classic test to detect median nerve irritation. Tinel's sign is performed by lightly tapping the skin over the flexor retinaculum to elicit a sensation of tingling or "pins and needles" in the median nerve distribution. Tinel's sign (pain or paresthesias of the median-innervated fingers with percussion over the median nerve), depending on the study, has 38–100% sensitivity and 55–100% specificity for the diagnosis of CTS.[7]
- Durkan test, carpal compression test, or applying firm pressure to the palm over the nerve for up to 30 seconds to elicit symptoms has also been proposed.[45][46]
- Hand elevation test The hand elevation test is performed by lifting both hands above the head, and if symptoms are reproduced in the median nerve distribution within 2 minutes, considered positive. The hand elevation test has higher sensitivity and specificity than Tinel's test, Phalen's test, and carpal compression test. Chi-square statistical analysis has shown the hand elevation test to be as effective, if not better than, Tinel's test, Phalen's test, and carpal compression test.[47]
As a note, a person with true carpal tunnel syndrome (entrapment of the median nerve within the carpal tunnel) will not have any sensory loss over the thenar eminence (bulge of muscles in the palm of hand and at the base of the thumb). This is because the palmar branch of the median nerve, which innervates that area of the palm, branches off of the median nerve and passes over the carpal tunnel.[48] This feature of the median nerve can help separate carpal tunnel syndrome from thoracic outlet syndrome, or pronator teres syndrome.
Other conditions may also be misdiagnosed as carpal tunnel syndrome. Thus, if history and physical examination suggest CTS, patients will sometimes be tested electrodiagnostically with nerve conduction studies and electromyography. The role of confirmatory nerve conduction studies is controversial.[7] The goal of electrodiagnostic testing is to compare the speed of conduction in the median nerve with conduction in other nerves supplying the hand. When the median nerve is compressed, as in CTS, it will conduct more slowly than normal and more slowly than other nerves. There are many electrodiagnostic tests used to make a diagnosis of CTS, but the most sensitive, specific, and reliable test is the Combined Sensory Index (also known as the Robinson index).[49] Electrodiagnosis rests upon demonstrating impaired median nerve conduction across the carpal tunnel in context of normal conduction elsewhere. Compression results in damage to the myelin sheath and manifests as delayed latencies and slowed conduction velocities [32] However, normal electrodiagnostic studies do not preclude the presence of carpal tunnel syndrome, as a threshold of nerve injury must be reached before study results become abnormal and cut-off values for abnormality are variable.[43] Carpal tunnel syndrome with normal electrodiagnostic tests is very, very mild at worst.
Imaging
The role of MRI or ultrasound imaging in the diagnosis of carpal tunnel syndrome is unclear.[50][51][52] Their routine use is not recommended.[3] MRI has high sensitivity but low specificity to CTS. High signal intensity would show accumulation of axonal transportation, myelin sheath degeneration or oedema.[53]
Differential diagnosis
There are few disorders on the differential diagnosis for carpal tunnel syndrome. Cervical radiculopathy can be mistaken for carpal tunnel syndrome since it can also cause abnormal or painful sensations in the hands and wrist.[7] In contrast to carpal tunnel syndrome, the symptoms of cervical radiculopathy usually begins in the neck and travels down the affected arm and may be worsened by neck movement.[7] Electromyography and imaging of the cervical spine can help to differentiate cervical radiculopathy from carpal tunnel syndrome if the diagnosis is unclear.[7] Carpal tunnel syndrome is sometimes applied as a label to anyone with pain, numbness, swelling, or burning in the radial side of the hands or wrists. When pain is the primary symptom, carpal tunnel syndrome is unlikely to be the source of the symptoms.[26] As a whole, the medical community is not currently embracing or accepting trigger point theories due to lack of scientific evidence supporting their effectiveness.
Prevention
There is little or no data to support the concept that activity adjustment prevents carpal tunnel syndrome.[54] The evidence for wrist rest is debated.[55] There is also little research supporting that ergonomics is related to CTS.[56] Due to risk factors for hand and wrist dysfunction being multifactorial and very complex it is difficult to assess the true physical factors of CTS.[57]
Biological factors such as genetic predisposition and anthropometric features had significantly stronger causal association with carpal tunnel syndrome than occupational/environmental factors such as repetitive hand use and stressful manual work.[54] This suggests that carpal tunnel syndrome might not be preventable simply by avoiding certain activities or types of work/activities.
Treatment
Generally accepted treatments include: physiotherapy, steroids either orally or injected locally, splinting, and surgical release of the transverse carpal ligament.[58] Limited evidence suggests that gabapentin is no more effective than placebo for CTS treatment.[7] There is insufficient evidence for therapeutic ultrasound, yoga, acupuncture, low level laser therapy, vitamin B6, and exercise.[7][58] Change in activity may include avoiding activities that worsen symptoms.[16]
The American Academy of Orthopedic Surgeons recommends proceeding conservatively with a course of nonsurgical therapies tried before release surgery is considered.[59] A different treatment should be tried if the current treatment fails to resolve the symptoms within 2 to 7 weeks. Early surgery with carpal tunnel release is indicated where there is evidence of median nerve denervation or a person elects to proceed directly to surgical treatment.[59] Recommendations may differ when carpal tunnel syndrome is found in association with the following conditions: diabetes mellitus, coexistent cervical radiculopathy, hypothyroidism, polyneuropathy, pregnancy, rheumatoid arthritis, and carpal tunnel syndrome in the workplace.[59]
Splints

The importance of wrist braces and splints in the carpal tunnel syndrome therapy is known, but many people are unwilling to use braces. In 1993, The American Academy of Neurology recommend a non-invasive treatment for the CTS at the beginning (except for sensitive or motor deficit or grave report at EMG/ENG): a therapy using splints was indicated for light and moderate pathology.[60] Current recommendations generally don't suggest immobilizing braces, but instead activity modification and non-steroidal anti-inflammatory drugs as initial therapy, followed by more aggressive options or specialist referral if symptoms do not improve.[61][62]
Many health professionals suggest that, for the best results, one should wear braces at night. When possible, braces can be worn during the activity primarily causing stress on the wrists.[63][64] The brace should not generally be used during the day as wrist activity is needed to keep the wrist from becoming stiff and to prevent muscles from weakening.[65]
Corticosteroids
Corticosteroid injections can be effective for temporary relief from symptoms while a person develops a long-term strategy that fits their lifestyle.[66] This form of treatment is thought to reduce discomfort in those with CTS due to its ability to decrease median nerve swelling.[7] The use of ultrasound while performing the injection is more expensive but leads to faster resolution of CTS symptoms.[7] The injections are done under local anesthesia.[67][68] This treatment is not appropriate for extended periods, however. In general, local steroid injections are only used until more definitive treatment options can be used. Corticosteroid injections do not appear to be very effective for slowing disease progression.[7]
Surgery
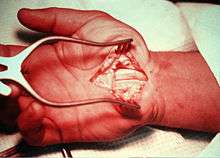
Release of the transverse carpal ligament is known as "carpal tunnel release" surgery. It is recommended when there is static (constant, not just intermittent) numbness, muscle weakness, or atrophy, and when night-splinting or other conservative interventions no longer control intermittent symptoms.[69] The surgery may be done with local[70][71][72] or regional anesthesia[73] with[74] or without[71] sedation, or under general anesthesia.[72][73] In general, milder cases can be controlled for months to years, but severe cases are unrelenting symptomatically and are likely to result in surgical treatment.[75]
Surgery is more beneficial in the short term to alleviate symptoms (up to six months) than wearing an orthosis for a minimum of 6 weeks. However, surgery and wearing a brace resulted in similar symptom relief in the long term (12–18 month outcomes).[76]
Physical therapy
An evidence based guideline produced by the American Academy of Orthopedic Surgeons assigned various grades of recommendation to physical therapy and other nonsurgical treatments.[77] One of the primary issues with physiotherapy is that it attempts to reverse (often) years of pathology inside the carpal tunnel. Practitioners caution that any physiotherapy such as myofascial release may take weeks of persistent application to effectively manage carpal tunnel syndrome.[78]
Again, some claim that pro-active ways to reduce stress on the wrists, which alleviates wrist pain and strain, involve adopting a more ergonomic work and life environment. For example, some have claimed that switching from a QWERTY computer keyboard layout to a more optimised ergonomic layout such as Dvorak was commonly cited as beneficial in early CTS studies; however, some meta-analyses of these studies claim that the evidence that they present is limited.[79][80]
Tendon and nerve gliding exercises appear to be useful in carpal tunnel syndrome.[81]
Prognosis
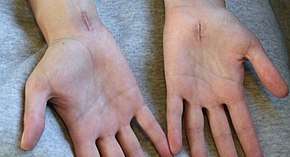
Most people relieved of their carpal tunnel symptoms with conservative or surgical management find minimal residual or "nerve damage".[82] Long-term chronic carpal tunnel syndrome (typically seen in the elderly) can result in permanent "nerve damage", i.e. irreversible numbness, muscle wasting, and weakness. Those that undergo a carpal tunnel release are nearly twice as likely as those not having surgery to develop trigger thumb in the months following the procedure.[83]
While outcomes are generally good, certain factors can contribute to poorer results that have little to do with nerves, anatomy, or surgery type. One study showed that mental status parameters or alcohol use yields much poorer overall results of treatment.[84]
Recurrence of carpal tunnel syndrome after successful surgery is rare.[85]
Epidemiology

Carpal tunnel syndrome is estimated to affect one out of ten people during their lifetime and is the most common nerve compression syndrome.[7] It accounts for about 90% of all nerve compression syndromes.[86] In the U.S., 5% of people have the effects of carpal tunnel syndrome. Caucasians have the highest risk of CTS compared with other races such as non-white South Africans.[87] Women suffer more from CTS than men with a ratio of 3:1 between the ages of 45–60 years. Only 10% of reported cases of CTS are younger than 30 years.[87] Increasing age is a risk factor. CTS is also common in pregnancy.[7]
Occupational
As of 2010, 8% of U.S. workers reported ever having carpal tunnel syndrome and 4% reported carpal tunnel syndrome in the past 12 months. Prevalence rates for carpal tunnel syndrome in the past 12 months were higher among females than among males; among workers aged 45–64 than among those aged 18–44. Overall, 67% of current carpal tunnel syndrome cases among current/recent workers were reportedly attributed to work by health professionals, indicating that the prevalence rate of work-related carpal tunnel syndrome among workers was 2%, and that there were approximately 3.1 million cases of work-related carpal tunnel syndrome among U.S. workers in 2010. Among current carpal tunnel syndrome cases attributed to specific jobs, 24% were attributed to jobs in the manufacturing industry, a proportion 2.5 times higher than the proportion of current/recent workers employed in the manufacturing industry, suggesting that jobs in this industry are associated with an increased risk of work-related carpal tunnel syndrome.[88]
History
The condition known as carpal tunnel syndrome had major appearances throughout the years but it was most commonly heard of in the years following World War II.[9] Individuals who had suffered from this condition have been depicted in surgical literature for the mid-19th century.[9] In 1854, Sir James Paget was the first to report median nerve compression at the wrist in two cases.[89][90]
The first to notice the association between the carpal ligament pathology and median nerve compression appear to have been Pierre Marie and Charles Foix in 1913.[91] They described the results of a postmortem of an 80-year-old man with bilateral carpal tunnel syndrome. They suggested that division of the carpal ligament would be curative in such cases. Putman had previously described a series of 37 patients and suggested a vasomotor origin.[92] The association between the thenar muscle atrophy and compression was noted in 1914.[93] The name 'carpal tunnel syndrome' appears to have been coined by Moersch in 1938.[94]
In the early 20th century there were various cases of median nerve compression underneath the transverse carpal ligament.[90] Physician Dr. George S. Phalen of the Cleveland Clinic identified the pathology after working with a group of patients in the 1950s and 1960s.[95][96]
- Treatment
Paget described two cases of carpal tunnel syndrome. The first was due to an injury where a cord had been wrapped around a man's wrist. The second was due to a distal radial fracture. For the first case Paget performed an amputation of the hand. For the second case Paget recommended a wrist splint – a treatment that is still in use today. Surgery for this condition initially involved the removal of cervical ribs despite Marie and Foix's suggested treatment. In 1933 Sir James Learmonth outlined a method of decompression of the nerve at the wrist.[97] This procedure appears to have been pioneered by the Canadian surgeons Herbert Galloway and Andrew MacKinnon in 1924 in Winnipeg but was not published.[98] Endoscopic release was described in 1988.[99]
References
- Burton, C; Chesterton, LS; Davenport, G (May 2014). "Diagnosing and managing carpal tunnel syndrome in primary care". The British Journal of General Practice. 64 (622): 262–3. doi:10.3399/bjgp14x679903. PMC 4001168. PMID 24771836.
- "Carpal Tunnel Syndrome Fact Sheet". National Institute of Neurological Disorders and Stroke. January 28, 2016. Archived from the original on 3 March 2016. Retrieved 4 March 2016.
- American Academy of Orthopaedic Surgeons (February 29, 2016). "Management of Carpal Tunnel Syndrome Evidence-Based Clinical Practice Guideline". Cite journal requires
|journal=(help) - Osterman, M; Ilyas, AM; Matzon, JL (October 2012). "Carpal tunnel syndrome in pregnancy". The Orthopedic Clinics of North America. 43 (4): 515–20. doi:10.1016/j.ocl.2012.07.020. PMID 23026467.
- Lozano-Calderón, S; Anthony, S; Ring, D (April 2008). "The quality and strength of evidence for etiology: example of carpal tunnel syndrome". The Journal of Hand Surgery. 33 (4): 525–38. doi:10.1016/j.jhsa.2008.01.004. PMID 18406957.
- Bickel, KD (January 2010). "Carpal tunnel syndrome". The Journal of Hand Surgery. 35 (1): 147–52. doi:10.1016/j.jhsa.2009.11.003. PMID 20117319.
- Padua, L; Coraci, D; Erra, C; Pazzaglia, C; Paolasso, I; Loreti, C; Caliandro, P; Hobson-Webb, LD (November 2016). "Carpal tunnel syndrome: clinical features, diagnosis, and management". Lancet Neurology (Review). 15 (12): 1273–84. doi:10.1016/S1474-4422(16)30231-9. PMID 27751557.
- Shiri, R (December 2014). "Hypothyroidism and carpal tunnel syndrome: a meta-analysis". Muscle & Nerve. 50 (6): 879–83. doi:10.1002/mus.24453. PMID 25204641.
- Amadio, Peter C. (2007). "History of carpal tunnel syndrome". In Luchetti, Riccardo; Amadio, Peter C. (eds.). Carpal Tunnel Syndrome. Berlin: Springer. pp. 3–9. ISBN 978-3-540-22387-0.
- "Carpal tunnel syndrome – Symptoms". NHS Choices. Archived from the original on 2016-05-24. Retrieved 2016-05-21. Page last reviewed: 18/09/2014
- Atroshi, I.; Gummesson, C; Johnsson, R; Ornstein, E; Ranstam, J; Rosén, I (1999). "Prevalence of Carpal Tunnel Syndrome in a General Population". JAMA. 282 (2): 153–158. doi:10.1001/jama.282.2.153. PMID 10411196.
- "Carpal Tunnel Syndrome Information Page". National Institute of Neurological Disorders and Stroke. December 28, 2010. Archived from the original on December 22, 2010.
- Netter, Frank (2011). Atlas of Human Anatomy (5th ed.). Philadelphia, PA: Saunders Elsevier. pp. 412, 417, 435. ISBN 978-0-8089-2423-4.
- Sternbach, G (1999). "The carpal tunnel syndrome". Journal of Emergency Medicine. 17 (3): 519–23. doi:10.1016/S0736-4679(99)00030-X. PMID 10338251.
- Katz, Jeffrey N.; Simmons, Barry P. (2002). "Carpal Tunnel Syndrome". New England Journal of Medicine. 346 (23): 1807–12. doi:10.1056/NEJMcp013018. PMID 12050342. S2CID 27783521.
- "Carpal Tunnel Syndrome". American Academy of Orthopaedic Surgeons. December 2009. Archived from the original on 2011-09-27.
- Tiong, W. H. C.; Ismael, T.; Regan, P. J. (2005). "Two rare causes of carpal tunnel syndrome". Irish Journal of Medical Science. 174 (3): 70–8. doi:10.1007/BF03170208. PMID 16285343.
- Conceição, I; González-Duarte, A; Obici, L; Schmidt, HH; Simoneau, D; Ong, ML; Amass, L (March 2016). ""Red-flag" symptom clusters in transthyretin familial amyloid polyneuropathy". Journal of the Peripheral Nervous System : JPNS. 21 (1): 5–9. doi:10.1111/jns.12153. PMC 4788142. PMID 26663427.
- Ibrahim I.; Khan W. S.; Goddard N.; Smitham P. (2012). "Suppl 1: Carpal Tunnel Syndrome: A Review of the Recent Literature". The Open Orthopaedics Journal. 6: 69–76. doi:10.2174/1874325001206010069. PMC 3314870. PMID 22470412.
- Armstrong T., Chaffin D. (1979). "Capral tunnel syndrome and selected personal attributes". Journal of Occupational Medicine. 21 (7).
- Schuind F.; Ventura M.; Pasteels J. (1990). "Idiopathic carpal tunnel syndrome: Histologic study of flexor tendon synovium". The Journal of Hand Surgery. 15 (3): 497–503. doi:10.1016/0363-5023(90)90070-8. PMID 2348074.
- Wiberg, A; Ng, M; Schmid, AB; Smillie, RW; Baskozos, G; Holmes, MV; Künnapuu, K; Mägi, R; Bennett, DL; Furniss, D (4 March 2019). "A genome-wide association analysis identifies 16 novel susceptibility loci for carpal tunnel syndrome". Nature Communications. 10 (1): 1030. Bibcode:2019NatCo..10.1030W. doi:10.1038/s41467-019-08993-6. PMC 6399342. PMID 30833571.
- Derebery, J (2006). "Work-related carpal tunnel syndrome: the facts and the myths". Clinics in Occupational and Environmental Medicine. 5 (2): 353–67, viii. doi:10.1016/j.coem.2005.11.014 (inactive 2020-06-05). PMID 16647653.
- Office of Communications and Public Liaison (December 18, 2009). "National Institute of Neurological Disorders and Stroke". Archived from the original on March 3, 2016.
- Werner, Robert A. (2006). "Evaluation of Work-Related Carpal Tunnel Syndrome". Journal of Occupational Rehabilitation. 16 (2): 201–16. doi:10.1007/s10926-006-9026-3. PMID 16705490.
- Graham, B. (1 December 2008). "The Value Added by Electrodiagnostic Testing in the Diagnosis of Carpal Tunnel Syndrome". The Journal of Bone and Joint Surgery. 90 (12): 2587–2593. doi:10.2106/JBJS.G.01362. PMID 19047703.
- Cole, Donald C.; Hogg-Johnson, Sheilah; Manno, Michael; Ibrahim, Selahadin; Wells, Richard P.; Ferrier, Sue E.; Worksite Upper Extremity Research Group (2006). "Reducing musculoskeletal burden through ergonomic program implementation in a large newspaper". International Archives of Occupational and Environmental Health. 80 (2): 98–108. doi:10.1007/s00420-006-0107-6. PMID 16736193.
- Luckhaupt, Sara E.; Burris, Dara L. (24 June 2013). "How Does Work Affect the Health of the U.S. Population? Free Data from the 2010 NHIS-OHS Provides the Answers". National Institute for Occupational Safety and Health. Archived from the original on 18 January 2015. Retrieved 18 January 2015.
- Swanson, Naomi; Tisdale-Pardi, Julie; MacDonald, Leslie; Tiesman, Hope M. (13 May 2013). "Women's Health at Work". National Institute for Occupational Safety and Health. Archived from the original on 18 January 2015. Retrieved 21 January 2015.
- LOZANOCALDERON, S; PAIVA, A; RING, D (1 March 2008). "Patient Satisfaction After Open Carpal Tunnel Release Correlates With Depression". The Journal of Hand Surgery. 33 (3): 303–307. doi:10.1016/j.jhsa.2007.11.025. PMID 18343281.
- LOZANOCALDERON, S; ANTHONY, S; RING, D (1 April 2008). "The Quality and Strength of Evidence for Etiology: Example of Carpal Tunnel Syndrome". The Journal of Hand Surgery. 33 (4): 525–538. doi:10.1016/j.jhsa.2008.01.004. PMID 18406957.
- Scott, Kevin R.; Kothari, Milind J. (October 5, 2009). "Treatment of carpal tunnel syndrome". UpToDate.
- Stevens JC, Beard CM, O'Fallon WM, Kurland LT (1992). "Conditions associated with carpal tunnel syndrome". Mayo Clin Proc. 67 (6): 541–548. doi:10.1016/S0025-6196(12)60461-3. PMID 1434881.
- "Carpel Tunnel Syndrome in Acromegaly". Treatmentandsymptoms.com. Archived from the original on 2016-01-26. Retrieved 2011-10-05.
- Werner, Robert A.; Albers, James W.; Franzblau, Alfred; Armstrong, Thomas J. (1994). "The relationship between body mass index and the diagnosis of carpal tunnel syndrome". Muscle & Nerve. 17 (6): 632–6. doi:10.1002/mus.880170610. hdl:2027.42/50161. PMID 8196706.
- Wilbourn AJ, Gilliatt RW (1997). "Double-crush syndrome: a critical analysis". Neurology. 49 (1): 21–27. doi:10.1212/WNL.49.1.21. PMID 9222165.
- Lupski, James R.; Reid, Jeffrey G.; Gonzaga-Jauregui, Claudia; Rio Deiros, David; Chen, David C.Y.; Nazareth, Lynne; Bainbridge, Matthew; Dinh, Huyen; et al. (2010). "Whole-Genome Sequencing in a Patient with Charcot–Marie–Tooth Neuropathy". New England Journal of Medicine. 362 (13): 1181–91. doi:10.1056/NEJMoa0908094. PMC 4036802. PMID 20220177.
- Brooks, JJ; Schiller, JR; Allen, SD; Akelman, E (Oct 2003). "Biomechanical and anatomical consequences of carpal tunnel release". Clinical Biomechanics (Bristol, Avon). 18 (8): 685–93. doi:10.1016/S0268-0033(03)00052-4. PMID 12957554.
- Vella, JC; Hartigan, BJ; Stern, PJ (Jul–Aug 2006). "Kaplan's cardinal line". The Journal of Hand Surgery. 31 (6): 912–8. doi:10.1016/j.jhsa.2006.03.009. PMID 16843150.
- RH Gelberman; PT Hergenroeder; AR Hargens; GN Lundborg; WH Akeson (1 March 1981). "The carpal tunnel syndrome. A study of carpal canal pressures". The Journal of Bone and Joint Surgery. 63 (3): 380–383. doi:10.2106/00004623-198163030-00009. PMID 7204435. Archived from the original on 22 March 2009. Retrieved 19 November 2010.
- Norvell, Jeffrey G.; Steele, Mark (September 10, 2009). "Carpal Tunnel Syndrome". eMedicine. Archived from the original on August 3, 2010. Cite journal requires
|journal=(help) - Rempel, D; Evanoff B; Amadio PC; et al. (1998). "Consensus criteria for the classification of carpal tunnel syndrome in epidemiologic studies". Am J Public Health. 88 (10): 1447–1451. doi:10.2105/AJPH.88.10.1447. PMC 1508472. PMID 9772842.
- Graham, B; Regehr G; Naglie G; Wright JG (2006). "Development and validation of diagnostic criteria for carpal tunnel syndrome". Journal of Hand Surgery. 31A (6): 919–924. PMID 16886290.
- Cush JJ, Lipsky PE (2004). "Approach to articular and musculoskeletal disorders". Harrison's Principles of Internal Medicine (16th ed.). McGraw-Hill Professional. p. 2035. ISBN 978-0-07-140235-4.
- Gonzalezdelpino, J; Delgadomartinez, A; Gonzalezgonzalez, I; Lovic, A (1997). "Value of the carpal compression test in the diagnosis of carpal tunnel syndrome". The Journal of Hand Surgery: Journal of the British Society for Surgery of the Hand. 22 (1): 38–41. doi:10.1016/S0266-7681(97)80012-5. PMID 9061521.
- Durkan, JA (1991). "A new diagnostic test for carpal tunnel syndrome". The Journal of Bone and Joint Surgery. American Volume. 73 (4): 535–8. doi:10.2106/00004623-199173040-00009. PMID 1796937. S2CID 11545887.
- Ma H, Kim I (November 2012). "The diagnostic assessment of hand elevation test in carpal tunnel syndrome". Journal of Korean Neurosurgical Society. 52 (5): 472–5. doi:10.3340/jkns.2012.52.5.472. PMC 3539082. PMID 23323168.
- Netter, Frank (2011). Atlas of Human Anatomy (5th ed.). Philadelphia, PA: Saunders Elsevier. p. 447. ISBN 978-0-8089-2423-4.
- Robinson, L (2007). "Electrodiagnosis of Carpal Tunnel Syndrome". Physical Medicine and Rehabilitation Clinics of North America. 18 (4): 733–46. doi:10.1016/j.pmr.2007.07.008. PMID 17967362.
- Wilder-Smith, Einar P; Seet, Raymond C S; Lim, Erle C H (2006). "Diagnosing carpal tunnel syndrome—clinical criteria and ancillary tests". Nature Clinical Practice Neurology. 2 (7): 366–74. doi:10.1038/ncpneuro0216. PMID 16932587.
- Bland, Jeremy DP (2005). "Carpal tunnel syndrome". Current Opinion in Neurology. 18 (5): 581–5. doi:10.1097/01.wco.0000173142.58068.5a. PMID 16155444.
- Jarvik, J; Yuen, E; Kliot, M (2004). "Diagnosis of carpal tunnel syndrome: electrodiagnostic and MR imaging evaluation". Neuroimaging Clinics of North America. 14 (1): 93–102, viii. doi:10.1016/j.nic.2004.02.002. PMID 15177259.
- Zamborsky, Radoslav; Kokavec, Milan; Simko, Lukas; Bohac, Martin (2017-01-26). "Carpal Tunnel Syndrome: Symptoms, Causes and Treatment Options. Literature Reviev". Ortopedia, Traumatologia, Rehabilitacja. 19 (1): 1–8. doi:10.5604/15093492.1232629. ISSN 2084-4336. PMID 28436376.
- Lozano-Calderón, Santiago; Shawn Anthony; David Ring (April 2008). "The Quality and Strength of Evidence for Etiology: Example of Carpal Tunnel Syndrome". The Journal of Hand Surgery. 33 (4): 525–538. doi:10.1016/j.jhsa.2008.01.004. PMID 18406957.
- "Wrist Rests : OSH Answers". Canadian Centre for Occupational Health and Safety. Archived from the original on 2017-04-15. Retrieved 2017-04-14.
- Goodman, G (2014-12-08). Ergonomic interventions for computer users with cumulative trauma disorders. International handbook of occupational therapy interventions. 2nd ed. pp. 205–17. ISBN 978-3-319-08140-3.
- Kalliainen, Loree K. (2017). "Nonoperative Options for the Management of Carpal Tunnel Syndrome". Carpal Tunnel Syndrome and Related Median Neuropathies. Springer, Cham. pp. 109–124. doi:10.1007/978-3-319-57010-5_11. ISBN 9783319570082.
- Piazzini, DB; Aprile, I; Ferrara, PE; Bertolini, C; Tonali, P; Maggi, L; Rabini, A; Piantelli, S; Padua, L (Apr 2007). "A systematic review of conservative treatment of carpal tunnel syndrome". Clinical Rehabilitation. 21 (4): 299–314. doi:10.1177/0269215507077294. PMID 17613571.
- Clinical Practice Guideline on the Treatment of Carpal Tunnel Syndrome (PDF). American Academy of Orthopaedic Surgeons. September 2008. Archived from the original (PDF) on 2009-12-11. Retrieved 2010-06-27.
- American Academy of Neurology (2006). "Quality Standards Subcommittee: Practice parameter for carpal tunnel syndrome". Neurology. 43 (11): 2406–2409. doi:10.1212/wnl.43.11.2406. PMID 8232968.
- Katz, Jeffrey N.; Simmons, Barry P. (2002). "Carpal Tunnel Syndrome". New England Journal of Medicine. 346 (23): 1807–1812. doi:10.1056/NEJMcp013018. PMID 12050342. S2CID 27783521.
- Harris JS, ed. (1998). Occupational Medicine Practice Guidelines: evaluation and management of common health problems and functional recovery in workers. Beverly Farms, Mass.: OEM Press. ISBN 978-1-883595-26-5.
- Premoselli, S; Sioli, P; Grossi, A; Cerri, C (2006). "Neutral wrist splinting in carpal tunnel syndrome: a 3- and 6-months clinical and neurophysiologic follow-up evaluation of night-only splint therapy". Europa Medicophysica. 42 (2): 121–6. PMID 16767058.
- Michlovitz, SL (2004). "Conservative interventions for carpal tunnel syndrome". The Journal of Orthopaedic and Sports Physical Therapy. 34 (10): 589–600. doi:10.2519/jospt.2004.34.10.589. PMID 15552705.
- Institute for Quality and Efficiency in Health Care (November 16, 2017). Carpal tunnel syndrome: Wrist splints and hand exercises. Institute for Quality and Efficiency in Health Care (IQWiG).
- Marshall, Shawn C; Tardif, Gaetan; Ashworth, Nigel L; Marshall, Shawn C (2007). Marshall, Shawn C (ed.). "Local corticosteroid injection for carpal tunnel syndrome". Cochrane Database of Systematic Reviews (2): CD001554. doi:10.1002/14651858.CD001554.pub2. PMID 17443508.
- "Carpal Tunnel Steroid Injection". Medscape. Archived from the original on July 29, 2015. Retrieved July 9, 2015.
- "Carpal Tunnel Injection Information". EBSCO. Archived from the original on 2015-07-10 – via The Mount Sinai Hospital.
- Hui, A.C.F.; Wong, S.M.; Tang, A.; Mok, V.; Hung, L.K.; Wong, K.S. (2004). "Long-term outcome of carpal tunnel syndrome after conservative treatment". International Journal of Clinical Practice. 58 (4): 337–9. doi:10.1111/j.1368-5031.2004.00028.x. PMID 15161116.
- "Open Carpal Tunnel Surgery for Carpal Tunnel Syndrome". WebMD. Archived from the original on July 7, 2015. Retrieved July 9, 2015.
- al Youha, Sarah; Lalonde, Donald (May 2014). "Update/Review: Changing of Use of Local Anesthesia in the Hand". Plastic and Reconstructive Surgery Global Open. 2 (5): e150. doi:10.1097/GOX.0000000000000095. PMC 4174079. PMID 25289343.
- Nabhan A, Ishak B, Al-Khayat J, Steudel W-I (April 25, 2008). "Endoscopic Carpal Tunnel Release using a modified application technique of local anesthesia: safety and effectiveness". Journal of Brachial Plexus and Peripheral Nerve Injury. 3 (11): e35–e38. doi:10.1186/1749-7221-3-11. PMC 2383895. PMID 18439257.
- "AAOS Informed Patient Tutorial – Carpal Tunnel Release Surgery". The American Academy of Orthopaedic Surgeons. Archived from the original on July 19, 2015. Retrieved July 9, 2015.
- Lee J-J, Hwang SM, Jang JS, Lim SY, Heo D-H, Cho YJ (2010). "Remifentanil-Propofol Sedation as an Ambulatory Anesthesia for Carpal Tunnel Release". Journal of Korean Neurosurgical Society. 48 (5): 429–433. doi:10.3340/jkns.2010.48.5.429. PMC 3030083. PMID 21286480.
- Kouyoumdjian, JA; Morita, MP; Molina, AF; Zanetta, DM; Sato, AK; Rocha, CE; Fasanella, CC (2003). "Long-term outcomes of symptomatic electrodiagnosed carpal tunnel syndrome". Arquivos de Neuro-Psiquiatria. 61 (2A): 194–8. doi:10.1590/S0004-282X2003000200007. PMID 12806496.
- D'Angelo, Kevin; Sutton, Deborah; Côté, Pierre; Dion, Sarah; Wong, Jessica J.; Yu, Hainan; Randhawa, Kristi; Southerst, Danielle; Varatharajan, Sharanya (2015). "The Effectiveness of Passive Physical Modalities for the Management of Soft Tissue Injuries and Neuropathies of the Wrist and Hand: A Systematic Review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration". Journal of Manipulative and Physiological Therapeutics. 38 (7): 493–506. doi:10.1016/j.jmpt.2015.06.006. PMID 26303967.
- Keith, M. W.; Masear, V.; Chung, K. C.; Amadio, P. C.; Andary, M.; Barth, R. W.; Maupin, K.; Graham, B.; Watters, W. C.; Turkelson, C. M.; Haralson, R. H.; Wies, J. L.; McGowan, R. (4 January 2010). "American Academy of Orthopaedic Surgeons Clinical Practice Guideline on The Treatment of Carpal Tunnel Syndrome". The Journal of Bone and Joint Surgery. 92 (1): 218–219. doi:10.2106/JBJS.I.00642. PMC 6882524. PMID 20048116. S2CID 7604145.
- Siu, G.; Jaffee, J.D.; Rafique, M.; Weinik, M.M. (1 March 2012). "Osteopathic Manipulative Medicine for Carpal Tunnel Syndrome". The Journal of the American Osteopathic Association. 112 (3): 127–139. PMID 22411967.
- Lincoln, A; Vernick, JS; Ogaitis, S; Smith, GS; Mitchell, CS; Agnew, J (2000). "Interventions for the primary prevention of work-related carpal tunnel syndrome". American Journal of Preventive Medicine. 18 (4 Suppl): 37–50. doi:10.1016/S0749-3797(00)00140-9. PMID 10793280.
- Verhagen, Arianne P; Karels, Celinde C; Bierma-Zeinstra, Sita MA; Burdorf, Lex L; Feleus, Anita; Dahaghin, Saede SD; De Vet, Henrica CW; Koes, Bart W; Verhagen, Arianne P (2006). Verhagen, Arianne P (ed.). "Ergonomic and physiotherapeutic interventions for treating work-related complaints of the arm, neck or shoulder in adults". Cochrane Database of Systematic Reviews. 3 (3): CD003471. doi:10.1002/14651858.CD003471.pub3. PMID 16856010. (Retracted, see doi:10.1002/14651858.cd003471.pub4. If this is an intentional citation to a retracted paper, please replace
{{Retracted}}with{{Retracted|intentional=yes}}.) - Kim, SD (August 2015). "Efficacy of tendon and nerve gliding exercises for carpal tunnel syndrome: a systematic review of randomized controlled trials". Journal of Physical Therapy Science. 27 (8): 2645–8. doi:10.1589/jpts.27.2645. PMC 4563334. PMID 26357452.
- Olsen, K. M.; Knudson, D. V. (2001). "Change in Strength and Dexterity after Open Carpal Tunnel Release". International Journal of Sports Medicine. 22 (4): 301–3. doi:10.1055/s-2001-13815. PMID 11414675.
- King, Bradley A.; Stern, Peter J.; Kiefhaber, Thomas R. (2013). "The incidence of trigger finger or de Quervain's tendinitis after carpal tunnel release". Journal of Hand Surgery (European Volume). 38 (1): 82–3. doi:10.1177/1753193412453424. PMID 22791612.
- Katz, Jeffrey N.; Losina, Elena; Amick, Benjamin C.; Fossel, Anne H.; Bessette, Louis; Keller, Robert B. (2001). "Predictors of outcomes of carpal tunnel release". Arthritis & Rheumatism. 44 (5): 1184–93. doi:10.1002/1529-0131(200105)44:5<1184::AID-ANR202>3.0.CO;2-A. PMID 11352253.
- Ruch, DS; Seal, CN; Bliss, MS; Smith, BP (2002). "Carpal tunnel release: efficacy and recurrence rate after a limited incision release". Journal of the Southern Orthopaedic Association. 11 (3): 144–7. PMID 12539938.
- Ibrahim I.; Khan W. S.; Goddard N.; Smitham P. (2012). "Carpal Tunnel Syndrome: A Review of the Recent Literature". The Open Orthopaedics Journal. 6: 69–76. doi:10.2174/1874325001206010069. PMC 3314870. PMID 22470412.
- Ashworth, Nigel L. (December 4, 2008). "Carpal Tunnel Syndrome". eMedicine. Archived from the original on July 28, 2010. Cite journal requires
|journal=(help) - Luckhaupt SE, Dahlhamer JM, Ward BW, Sweeney MH, Sestito JP, Calvert GM (June 2013). "Prevalence and work-relatedness of carpal tunnel syndrome in the working population, United States, 2010 National Health Interview Survey". American Journal of Industrial Medicine. 56 (6): 615–24. doi:10.1002/ajim.22048. PMC 4557701. PMID 22495886.
- Paget J (1854) Lectures on surgical pathology. Lindsay & Blakinston, Philadelphia
- Fuller, David A. (September 22, 2010). "Carpal Tunnel Syndrome". eMedicine. Archived from the original on July 27, 2010. Cite journal requires
|journal=(help) - Marie P, Foix C (1913). "Atrophie isolée de l'éminence thenar d'origine névritique: role du ligament annulaire antérieur du carpe dans la pathogénie de la lésion". Rev Neurol. 26: 647–649.
- Putnam JJ (1880). "A series of cases of paresthesia, mainly of the hand, or periodic recurrence, and possibly of vaso-motor origin". Arch Med. 4: 147–162.
- Hunt JR (1914). "The neural atrophy of the muscle of the hand, without sensory disturbances". Rev Neurol Psych. 12: 137–148.
- Moersch FP (1938). "Median thenar neuritis". Proc Staff Meet Mayo Clin. 13: 220.
- Phalen GS, Gardner WJ, Lalonde AA (1950). "Neuropathy of the median nerve due to compression beneath the transverse carpal ligament". J Bone Joint Surg Am. 1: 109–112. doi:10.2106/00004623-195032010-00011. PMID 15401727.
- Gilliatt RW, Wilson TG (1953). "A pneumatic-tourniquet test in the carpal-tunnel syndrome". Lancet. 262 (6786): 595–597. doi:10.1016/s0140-6736(53)90327-4. PMID 13098011.
- Learmonth JR (1933). "The principle of decompression in the treatment of certain diseases of peripheral nerves". Surg Clin North Am. 13: 905–913.
- Amadio PC (1995). "The first carpal tunnel release?". J Hand Surg: British & European. 20 (1): 40–41. doi:10.1016/s0266-7681(05)80013-0. PMID 7759932.
- Chow JC (1989). "Endoscopic release of the carpal tunnel ligament: a new technique for carpal tunnel syndrome". Arthroscopy. 6 (4): 288–296. doi:10.1016/0749-8063(90)90058-l. PMID 2264896.
External links
| Classification | |
|---|---|
| External resources |