Hidradenitis suppurativa
Hidradenitis suppurativa (HS), also known as acne inversa, is a long-term skin disease characterized by the occurrence of inflamed and swollen lumps.[2][3] These are typically painful and break open, releasing fluid or pus.[3] The areas most commonly affected are the underarms, under the breasts, and groin.[1] Scar tissue remains after healing.[1]
| Hidradenitis suppurativa | |
|---|---|
| Other names | Acne inversa, acne conglobata, apocrine acne, Verneuil's disease, Velpeau’s disease[1] |
_in_axilla.jpg) | |
| Hidradenitis suppurativa (stage II) in the left armpit | |
| Specialty | Dermatology |
| Symptoms | Multiple inflamed and swollen skin lesions[2] |
| Usual onset | Young adulthood[2] |
| Duration | Long-term[2] |
| Types | Stage I, II, III[1] |
| Causes | Unknown[3] |
| Diagnostic method | Based on symptoms[2] |
| Differential diagnosis | Acne, acne conglobata, pilonidal cysts[2] |
| Treatment | Warm baths, laser therapy, surgery[2][4] |
| Medication | Antibiotics, immunosuppressive medication[2] |
| Frequency | 1–4% of people[2] |
| Deaths | Rare[1] |
The exact cause is usually unclear but believed to involve a combination of genetic and environmental factors.[3] About a third of people with the disease have an affected family member.[3] Other risk factors include obesity and smoking.[3] The condition is not infectious, related to hygiene, or the use of deodorant.[3][4] The underlying mechanism is believed to involve either a dysfunction of apocrine sweat glands or hair follicles.[1][3] Diagnosis is based on the symptoms.[2]
There is no known cure.[4] Warm baths may be tried in those with mild disease.[4] Cutting open the lesions to allow them to drain does not result in significant benefit.[2] While antibiotics are commonly used, evidence for their use is poor.[4] Immunosuppressive medication may also be tried.[2] In those with more severe disease, laser therapy or surgery to remove the affected skin may be carried out.[2] Rarely, a skin lesion may develop into skin cancer.[3]
It is estimated to affect between 1% and 4% of people.[2] Women have the condition about three times more often than men.[2] Onset is typically in young adulthood and may become less common after 50 years old.[2] It was first described some time between 1833 and 1839 by French anatomist Alfred Velpeau.[1][5]
Causes
The cause of hidradenitis suppurativa remains unknown, and experts disagree over proposed causes.[6] The condition probably results from a combination of genetic and environmental factors.
Lesions occur in any body areas with hair follicles, although areas such as the axilla, groin, and perianal region are more commonly involved. This theory includes most of the following potential indicators:[7]
- Post-pubescent individuals[8]
- Plugged apocrine (sweat) gland or hair follicle
- Excessive sweating
- Androgen dysfunction
- Genetic disorders that alter cell structure
- Patients with more advanced cases may find exercise intolerably painful, which may increase the rate of obesity among sufferers.
The historical understanding of the disease suggests dysfunctional apocrine glands[9] or dysfunctional hair follicles,[10] possibly triggered by a blocked gland, which creates inflammation, pain, and a swollen lesion.
Triggering factors
Several triggering factors should be taken into consideration:
- Obesity[11] is an exacerbating rather than a triggering factor,[12] through mechanical irritation, occlusion, and skin maceration.
- Tight clothing,[11] and clothing made of heavy, non-breathable materials.[13]
- Deodorants, depilation products, shaving of the affected area – their association with HS is still an ongoing debate amongst researchers.[14]
- Drugs, in particular oral contraceptive pills[15] and lithium.[16]
- Hot and especially humid climates[17] (dry and arid climates often cause remission).
Predisposing factors
- Genetic factors:[12] an autosomal dominant inheritance pattern has been proposed.[18]
- Endocrine factors: sex hormones, especially an excess of androgens, are thought to be involved, although the apocrine glands are not sensitive to these hormones.[19] Women often have outbreaks before their menstrual period and after pregnancy; HS severity usually decreases during pregnancy and after menopause.
Some cases have been found to result from mutations in the NCSTN, PSEN1 or PSENEN genes. The genes produce proteins that are all components of a complex called gamma- (γ-) secretase. This complex cuts apart (cleaves) many different proteins, which is an important step in several chemical signaling pathways. One of these pathways, known as Notch signaling, is essential for the normal maturation and division of hair follicle cells and other types of skin cells. Notch signaling is also involved in normal immune system function. Studies suggest that mutations in the NCSTN, PSEN1, or PSENEN gene impair Notch signaling in hair follicles. Although little is known about the mechanism, abnormal Notch signaling appears to promote the development of nodules and lead to inflammation in the skin.[20]
Diagnosis
Stages
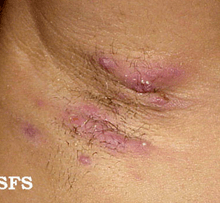

Hidradenitis suppurativa presents itself in three stages.[9][22] Due to the large spectrum of clinical severity and the severe impact on quality of life, a reliable method for evaluating HS severity is needed.
Hurley's staging system
The Hurley's staging system was the first classification system proposed, and is still in use for the classification of patients with skin diseases (i.e., psoriasis, HS, acne). Hurley separated patients into three groups based largely on the presence and extent of cicatrization and sinuses. It has been used as a basis for clinical trials in the past and is a useful basis to approach therapy for patients. These three stages are based on Hurley's staging system, which is simple and relies on the subjective extent of the diseased tissue the patient has. Hurley's three stages of hidradenitis suppurativa are:[23]
| Stage | Characteristics |
|---|---|
| I | Solitary or multiple isolated abscess formation without scarring or sinus tracts. (A few minor sites with rare inflammation; may be mistaken for acne.) |
| II | Recurrent abscesses, single or multiple widely separated lesions, with sinus tract formation. (Frequent inflammation restrict movement and may require minor surgery such as incision and drainage.) |
| III | Diffuse or broad involvement across a regional area with multiple interconnected sinus tracts and abscesses (Inflammation of sites to the size of golf balls, or sometimes baseballs; scarring develops, including subcutaneous tracts of infection – see fistula. Obviously, patients at this stage may be unable to function.) |
Sartorius staging system
The Sartorius staging system is more sophisticated than Hurley's. Sartorius et al. suggested that the Hurley system is not sophisticated enough to assess treatment effects in clinical trials during research. This classification allows for better dynamic monitoring of the disease severity in individual patients. The elements of this staging system are:[24]
- Anatomic regions involved (axilla, groin gluteal, or other region or inframammary region left or right)
- Number and types of lesions involved (abscesses, nodules, fistulas or sinuses, scars, points for lesions of all regions involved)
- The distance between lesions, in particular the longest distance between two relevant lesions (i.e., nodules and fistulas in each region or size if only one lesion present)
- The presence of normal skin in between lesions (i.e., if all lesions are clearly separated by normal skin)
Points are accumulated in each of the above categories, and added to give both a regional and total score. In addition, the authors recommend adding a visual analog scale for pain or using the dermatology life quality index (DLQI, or the 'skindex') when assessing HS.[25]
Treatment
Treatment depends upon presentation and severity of the disease. Due to the poorly studied nature of the disease, the effectiveness of the drugs and therapies listed below is unclear.[26] Possible treatments include the following:
Lifestyle
Warm baths may be tried in those with mild disease.[4] Weight loss and stopping smoking is also recommended.[2]
Medication
- Antibiotics: taken by mouth, these are used for their anti-inflammatory properties rather than to treat infection. Most effective is a combination of rifampicin and clindamycin given concurrently for 2–3 months. A few popular antibiotics include tetracycline, minocycline, and clindamycin.[27] Topical clindamycin has been shown to have an effect in double-blind placebo controlled studies.[28]
- Corticosteroid injections. Also known as intralesional steroids: can be particularly useful for localized disease, if the drug can be prevented from escaping via the sinuses.
- Antiandrogen therapy: hormonal therapy with antiandrogenic medications such as spironolactone, flutamide, cyproterone acetate, ethinylestradiol, finasteride, dutasteride, and metformin have been found to be effective in clinical studies.[29][30][31] However, the quality of available evidence is low and does not presently allow for robust evidence-based recommendations.[29][30]
- Intravenous or subcutaneous infusion of anti-inflammatory (TNF inhibitors; anti-TNF-alpha) drugs such as infliximab, and etanercept.[32] This use of these drugs is not currently Food and Drug Administration (FDA) approved and is somewhat controversial, so may not be covered by insurance.
- TNF inhibitor: Studies have supported that various TNF inhibitors have a positive effect on HS lesions.[33] Specifically adalimumab at weekly intervals is useful.[34]
- Topical isotretinoin is usually ineffective in people with HS and is more commonly known as a medication for the treatment of acne vulgaris. Individuals affected by HS who responded to isotretinoin treatment tended to have milder cases of the condition.[35]
Surgery
When the process becomes chronic, wide surgical excision is the procedure of choice. Wounds in the affected area do not heal by secondary intention, and immediate or delayed application of a split-thickness skin graft is an option.[7] Another option is covering the defect with a so-called perforator flap. With this technique the (mostly totally excised) defect is covered with living tissue 'stolen' from the area nearby. For example, the axilla with a fully excised defect of 15 × 7 cm can be covered with a so-called TAP flap (thoracodorsal artery perforator flap)
Laser hair removal
The 1064 nanometer wavelength laser for hair removal may aid in the treatment of HS.[36] A randomized control study has shown improvement in HS lesions with the use of an Nd:YAG laser.[37]
Prognosis
In stage III disease, as classified by the Hurley's staging system, fistulae left undiscovered, undiagnosed, or untreated, can rarely lead to the development of squamous cell carcinoma in the anus or other affected areas.[38][39] Other stage III chronic sequelae may also include anemia, multilocalized infections, amyloidosis, and arthropathy. Stage III complications have been known to lead to sepsis, but clinical data is still uncertain.
Potential complications
- Contractures and reduced mobility of the lower limbs and axillae due to fibrosis and scarring occur. Severe lymphedema may develop in the lower limbs.
- Local and systemic infections (meningitis, bronchitis, pneumonia, etc.), are seen, which may even progress to sepsis.
- Interstitial keratitis
- Anal, rectal, or urethral fistulae[40]
- Normochromic or hypochromic anemia[41]
- People with HS may be at increased risk for autoimmune disorders including ankylosing spondylitis, rheumatoid arthritis, and psoriatic arthritis.[42]
- Squamous cell carcinoma: this has been found on rare occasions in chronic hidradenitis suppurativa of the anogenital region.[43] The mean time to the onset of this type of lesion is 10 years or more and the tumors are usually highly aggressive.
- Tumors of the lung and oral cavity, probably related to the high level of smoking among these patients, and liver cancer.[44]
- Hypoproteinemia and amyloidosis, which can lead to kidney failure and death[45]
- Seronegative and usually asymmetric arthropathy: pauciarticular arthritis, polyarthritis/polyarthralgia syndrome[46]
History
- From 1833 to 1839 in a series of three publications, Velpeau identified and described a disease we now know as hidradenitis suppurativa.[47]
- In 1854, Verneuil described hidradenitis suppurativa as hidrosadénite Phlegmoneuse. This is how HS obtained its alternate name "Verneuil's disease".[48]
- In 1922, Schiefferdecker hypothesized a pathogenic link between "acne inversa" and human sweat glands.[49]
- In 1956, Pillsbury et al.[50] coined the term follicular occlusion triad for the common association of hidradenitis suppurativa, acne conglobata and dissecting cellulitis of the scalp. Modern clinical research still employs Pillsbury's terminology for these conditions' descriptions.[51]
- In 1975, Plewig and Kligman, following Pillsbury's research path, modified the "acne triad", replacing it with the "acne tetrad: acne triad, plus pilonidal sinus".[52] Plewig and Kligman's research follows in Pillsbury's footsteps, offering explanations of the symptoms associated with hidradenitis suppurativa.
- In 1989, Plewig and Steger's research led them to rename hidradenitis suppurativa, calling it "acne inversa" – which is not still used today in medical terminology, although some individuals still use this outdated term.[53]
A surgeon from Paris, Velpeau described an unusual inflammatory process with formation of superficial axillary, submammary, and perianal abscesses, in a series of three publications from 1833 to 1839. One of his colleagues also located in Paris, named Verneuil, coined the term hidrosadénite phlegmoneuse about 15 years later. This name for the disease reflects the former pathogenetic model of acne inversa, which is considered inflammation of sweat glands as the primary cause of hidradenitis suppurativa. In 1922, Schiefferdecker suspected a pathogenic association between acne inversa and apocrine sweat glands. In 1956 Pillsbury postulated follicular occlusion as the cause of acne inversa, which they grouped together with acne conglobata and perifolliculitis capitis abscendens et suffodiens ("dissecting cellulitis of the scalp") as the "acne triad". Plewig and Kligman added another element to their acne triad, pilonidal sinus. Plewig et al. noted that this new "acne tetrad" includes all the elements found in the original "acne triad", in addition to a fourth element, pilonidal sinus. In 1989, Plewig and Steger introduced the term "acne inversa", indicating a follicular source of the disease and replacing older terms such as "Verneuil disease".
| Author | Year | Findings |
|---|---|---|
| Velpeau | 1839 | First description of the hidradenitis suppurativa |
| Verneuil | 1854 | "Hidrosadénite phlegmoneuse" |
| Pillsbury | 1956 | Acne triad (hidradenitis suppurativa, perifolliculitis capitis abscendens et suffodiens, acne congoblata) |
| Plewig & Kligman | 1975 | Acne tetrad (acne triad + pilonidal sinus) |
| Plewig & Steger | 1989 | Acne inversa |
Other names
Hidradenitis suppurativa has been referred to by multiple names in the literature, as well as in various cultures. Some of these are also used to describe different diseases, or specific instances of this disease.[22]
- Acne conglobata – not really a synonym – this is a similar process but in classic acne areas of chest and back
- Acne inversa – a proposed new term[54][55] which has not gained widespread favor.[56]
- Apocrine acne – an outdated term based on the disproven concept that apocrine glands are primarily involved, though many do suffer with apocrine gland infection
- Apocrinitis – another outdated term based on the same thesis
- Fox-den disease – a term not used in medical literature, based on the deep fox den–like sinuses
- Hidradenitis supportiva – a misspelling
- Pyodermia fistulans significa – now considered archaic
- Verneuil's disease – recognizing the surgeon whose name is most often associated with the disorder as a result of his 1854–1865 studies[57]
Histology
| Author | Year | Major Features |
|---|---|---|
| Plewig & Steger[53] | 1989 | Initial hyperkeratosis of the follicular infundibulum. Bacterial super-infection and follicle rupture. Granulomatous inflammatory reaction of the connective tissue. Apocrine and eccrine sweat glands secondarily involved. |
| Yu & Cook[58] | 1990 | Cysts and sinus tracts lined with epithelium, in part with hair shafts. Inflammation of apocrine sweat glands only if eccrine sweat glands and hair follicles are also inflamed. |
| Boer & Weltevreden[59] | 1996 | Primary inflammation of the follicular infundibulum. Apocrine sweat glands are secondarily involved. |
Terminology
Although hidradenitis suppurativa is often referred to as acne inversa, it is not a form of acne and lacks the core defining features of acne such as the presence of closed comedones and increased sebum production.[60]
References
- "Hidradenitis Suppurativa". NORD (National Organization for Rare Disorders). 2012. Archived from the original on 19 February 2017. Retrieved 26 October 2017.
- Jemec GB (January 2012). "Clinical practice. Hidradenitis suppurativa". The New England Journal of Medicine. 366 (2): 158–64. doi:10.1056/NEJMcp1014163. PMID 22236226.
- "Hidradenitis suppurativa". Genetics Home Reference. December 2013. Archived from the original on 5 September 2017. Retrieved 27 October 2017.
- "Hidradenitis suppurativa". rarediseases.info.nih.gov. 2017. Archived from the original on 28 July 2017. Retrieved 27 October 2017.
- Jemec G, Revuz J, Leyden JJ (2006). Hidradenitis Suppurativa. Springer Science & Business Media. p. 5. ISBN 9783540331018. Archived from the original on 28 October 2017.
- Medline Plus (2012). "Hidradenitis suppurativa". U.S. National Library of Medicine. Archived from the original on 16 September 2012. Retrieved 19 September 2012.
- Schawartz's principles of surgery, 8th edition, self assessment an board review, chapter 15, the skin and subcutaneous tissue, question 16
- Mayo Clinic Staff (2012). "Definition". Mayo Clinic. Archived from the original on 10 September 2012. Retrieved 19 September 2012.
- DermNet acne/hidradenitis-suppurativa
- "HSF – What is Hidradenitis Suppurativa? What is HS?". Archived from the original on 6 July 2007. Retrieved 8 July 2007.
- Slade DE, Powell BW, Mortimer PS (July 2003). "Hidradenitis suppurativa: pathogenesis and management". British Journal of Plastic Surgery. 56 (5): 451–61. doi:10.1016/S0007-1226(03)00177-2. PMID 12890458.
- Jemec GBE. Body weight in hidradenitis suppurativa. In: Marks R, Plewig G, editors. Acne and Related disorders. London: Martin Dunitz; 1989. pp. 375–6.
- König A, Lehmann C, Rompel R, Happle R (1999). "Cigarette smoking as a triggering factor of hidradenitis suppurativa". Dermatology. 198 (3): 261–4. doi:10.1159/000018126. PMID 10393449.
- Morgan WP, Hughes LE (December 1979). "The distribution, size and density of the apocrine glands in hidradenitis suppuritiva". The British Journal of Surgery. 66 (12): 853–6. doi:10.1002/bjs.1800661206. PMID 509057.
- Stellon AJ, Wakeling M (January 1989). "Hidradenitis suppurativa associated with use of oral contraceptives". BMJ. 298 (6665): 28–9. doi:10.1136/bmj.298.6665.28. PMC 1835363. PMID 2492847.
- Gupta AK, Knowles SR, Gupta MA, Jaunkalns R, Shear NH (February 1995). "Lithium therapy associated with hidradenitis suppurativa: case report and a review of the dermatologic side effects of lithium". Journal of the American Academy of Dermatology. 32 (2 Pt 2): 382–6. doi:10.1016/0190-9622(95)90410-7. PMID 7829746.
- Hidradenitis Suppurativa at eMedicine
- Von Der Werth JM, Williams HC, Raeburn JA (May 2000). "The clinical genetics of hidradenitis suppurativa revisited". The British Journal of Dermatology. 142 (5): 947–53. doi:10.1046/j.1365-2133.2000.03476.x. PMID 10809853.
- Barth JH, Kealey T (October 1991). "Androgen metabolism by isolated human axillary apocrine glands in hidradenitis suppurativa". The British Journal of Dermatology. 125 (4): 304–8. doi:10.1111/j.1365-2133.1991.tb14162.x. PMID 1954117.
- Reference, Genetics Home. "hidradenitis suppurativa". Genetics Home Reference. Archived from the original on 5 September 2017. Retrieved 5 September 2017.
- Giang, Jenny; Seelen, Marc A. J.; van Doorn, Martijn B. A.; Rissmann, Robert; Prens, Errol P.; Damman, Jeffrey (2018). "Complement Activation in Inflammatory Skin Diseases". Frontiers in Immunology. 9. doi:10.3389/fimmu.2018.00639. ISSN 1664-3224. PMC 5911619. PMID 29713318.
- "HS-USA :: What is Hidradenitis Suppurativa?". Archived from the original on 17 June 2013. Retrieved 20 July 2013.
- Hurley HJ. Axillary hyperhidrosis, apocrine bromhidrosis, hidradenitis suppurativa, and familial benign pemphigus: surgical approach. In: Roenigk RK, Roenigk HH, editors. Dermatologic surgery. Marcel Dekker, New York, 1989, pp. 729–739.
- Sartorius K, Lapins J, Emtestam L, Jemec GB (July 2003). "Suggestions for uniform outcome variables when reporting treatment effects in hidradenitis suppurativa". The British Journal of Dermatology. 149 (1): 211–3. doi:10.1046/j.1365-2133.2003.05390.x. PMID 12890229.
- Wolkenstein P, Loundou A, Barrau K, Auquier P, Revuz J (April 2007). "Quality of life impairment in hidradenitis suppurativa: a study of 61 cases". Journal of the American Academy of Dermatology. 56 (4): 621–3. doi:10.1016/j.jaad.2006.08.061. PMID 17097366.
- Ingram JR, Woo PN, Chua SL, Ormerod AD, Desai N, Kai AC, et al. (May 2016). "Interventions for hidradenitis suppurativa: a Cochrane systematic review incorporating GRADE assessment of evidence quality". The British Journal of Dermatology. 174 (5): 970–8. doi:10.1111/bjd.14418. PMC 5021164. PMID 26801356.
- Scheinfeld N (April 2013). "Hidradenitis suppurativa: A practical review of possible medical treatments based on over 350 hidradenitis patients". Dermatology Online Journal. 19 (4): 1. PMID 24021361.
- Clemmensen OJ (June 1983). "Topical treatment of hidradenitis suppurativa with clindamycin". International Journal of Dermatology. 22 (5): 325–8. doi:10.1111/j.1365-4362.1983.tb02150.x. PMID 6347922.
- Nikolakis, Georgios; Kyrgidis, Athanassios; Zouboulis, Christos C. (2019). "Is There a Role for Antiandrogen Therapy for Hidradenitis Suppurativa? A Systematic Review of Published Data". American Journal of Clinical Dermatology. 20 (4): 503–513. doi:10.1007/s40257-019-00442-w. ISSN 1175-0561. PMID 31073704.
- Goldburg, Samantha R.; Strober, Bruce E.; Payette, Michael J. (2019). "Part 2. Current and emerging treatments for hidradenitis suppurativa". Journal of the American Academy of Dermatology. doi:10.1016/j.jaad.2019.08.089. ISSN 0190-9622. PMID 31604100.
- Student, Sebastian; Hejmo, Tomasz; Poterała-Hejmo, Aleksandra; Leśniak, Aleksandra; Bułdak, Rafał (2020). "Anti-androgen hormonal therapy for cancer and other diseases". European Journal of Pharmacology. 866: 172783. doi:10.1016/j.ejphar.2019.172783. ISSN 0014-2999. PMID 31712062.
- Cusack C, Buckley C (April 2006). "Etanercept: effective in the management of hidradenitis suppurativa". The British Journal of Dermatology. 154 (4): 726–9. doi:10.1111/j.1365-2133.2005.07067.x. PMID 16536817.
- Haslund P, Lee RA, Jemec GB (November 2009). "Treatment of hidradenitis suppurativa with tumour necrosis factor-alpha inhibitors". Acta Dermato-Venereologica. 89 (6): 595–600. doi:10.2340/00015555-0747. PMID 19997689.
- Ingram JR (May 2017). "Interventions for Hidradenitis Suppurativa: Updated Summary of an Original Cochrane Review". JAMA Dermatology. 153 (5): 458–459. doi:10.1001/jamadermatol.2017.0432. PMID 28355440.
- Nickle SB, Peterson N, Peterson M (April 2014). "Updated Physician's Guide to the Off-label Uses of Oral Isotretinoin". The Journal of Clinical and Aesthetic Dermatology. 7 (4): 22–34. PMC 3990537. PMID 24765227.
- Scheinfeld N (April 2013). "Hidradenitis suppurativa: A practical review of possible medical treatments based on over 350 hidradenitis patients". Dermatology Online Journal. 19 (4): 1. PMID 24021361. Archived from the original on 6 March 2014. Retrieved 4 March 2014.
- Xu LY, Wright DR, Mahmoud BH, Ozog DM, Mehregan DA, Hamzavi IH (January 2011). "Histopathologic study of hidradenitis suppurativa following long-pulsed 1064-nm Nd:YAG laser treatment". Archives of Dermatology. 147 (1): 21–8. doi:10.1001/archdermatol.2010.245. PMID 20855672.
- Talmant JC, Bruant-Rodier C, Nunziata AC, Rodier JF, Wilk A (February 2006). "[Squamous cell carcinoma arising in Verneuil's disease: two cases and literature review]". Annales de Chirurgie Plastique et Esthetique (in French). 51 (1): 82–6. doi:10.1016/j.anplas.2005.11.002. PMID 16488526.
- Short KA, Kalu G, Mortimer PS, Higgins EM (September 2005). "Vulval squamous cell carcinoma arising in chronic hidradenitis suppurativa". Clinical and Experimental Dermatology. 30 (5): 481–3. doi:10.1111/j.1365-2230.2005.01875.x. PMID 16045671.
- Hurley HJJ. Apocrine glands. New York: McGraw Hill; 1979.
- Tennant F, Bergeron JR, Stone OJ, Mullins JF (August 1968). "Anemia associated with hidradenitis suppurativa". Archives of Dermatology. 98 (2): 138–40. doi:10.1001/archderm.98.2.138. PMID 5667225.
- Schneeweiss MC, Kim SC, Schneeweiss S, Rosmarin D, Merola JF (2020). "Risk of inflammatory arthritis after a new diagnosis of hidradenitis suppurativa". JAMA Dermatology. 156: 342. doi:10.1001/jamadermatol.2019.4590.
- Williams ST, Busby RC, DeMuth RJ, Nelson H (May 1991). "Perineal hidradenitis suppurativa: presentation of two unusual complications and a review". Annals of Plastic Surgery. 26 (5): 456–62. doi:10.1097/00000637-199105000-00008. PMID 1952719.
- Lapins J, Ye W, Nyrén O, Emtestam L (June 2001). "Incidence of cancer among patients with hidradenitis suppurativa". Archives of Dermatology. 137 (6): 730–4. PMID 11405761.
- Moschella SL (October 1966). "Hidradenitis suppurativa. Complications resulting in death". JAMA. 198 (1): 201–3. doi:10.1001/jama.198.1.201. PMID 5953172.
- Vasey FB, Fenske NA, Clement GB, Bridgeford PH, Germain BF, Espinoza LR (1984). "Immunological studies of the arthritis of acne conglobata and hidradenitis suppurativa". Clinical and Experimental Rheumatology. 2 (4): 309–11. PMID 6241861.
- Velpeau A. Aissele. In: Bechet Jeune Z: Dictionnaire de médecine, on Repertoire Générale des Sciences Medicals sous le Rapport Theorique et Pratique. 1839.
- Verneuil AS (1854). "Etudes sur les tumeurs de la peau et quelques maladies de glandes sudoripares" [Studies on skin tumors; some diseases of the sweat glands]. Archives of General Medicine (in French). 94: 693–705.
- Schiefferdecker B (1922). Die Hautdrüsen der Menschen und der Säugetiere, ihre histologische und rassenanatomische Bedeutung sowie die muscularis sexualis [The skin glands of humans and mammals, their histological and anatomical racial meaning and muscularis sexualis]. Stuttgart: Schweizerbart E.
- Pillsbury DM, Shelley WB, Kligmann AM (1956). "Bacterial infections of the skin". In Pillsbury DM (ed.). Dermatoloy (1st ed.). Philadelphia. pp. 482–9.
- Triads in Dermatology; Prachi G Agrawal, Uday S Khopkar, [...], and Sunil N Mishra; J Dermatol. 2013 Sep–Oct; 58(5): 346–351
- Plewig G, Kligman AM (1975). "Acne Conglobata". In Plewig G, Kligman AM (eds.). Acne: Morphogenesis and Treatment. pp. 168–203. doi:10.1007/978-3-642-96246-2_11. ISBN 978-3-642-96246-2.
- Plewig G, Steger M (1989). "Acne inversa (alias acne triad, acne tetrad or hidradenitis suppurativa)". In Marks R, Plewig G (eds.). Acne and Related Disorders. London: Martin Dunitz. pp. 345–57.
- Sellheyer K, Krahl D (July 2005). ""Hidradenitis suppurativa" is acne inversa! An appeal to (finally) abandon a misnomer". International Journal of Dermatology. 44 (7): 535–40. doi:10.1111/j.1365-4632.2004.02536.x. PMID 15985019.
- Bazex J, Bayle P, San B (March 2007). "Hidradenitis suppurativa is acne inversa". International Journal of Dermatology. 46 (3): 330, author reply 330–2. doi:10.1111/j.1365-4632.2007.02872.x. PMID 17343599.
- Scheinfeld N (December 2006). "Hidradenitis should not be renamed acne inversa". Dermatology Online Journal. 12 (7): 6. PMID 17459292.
- Verneuil AS (1854). "Etudes sur les tumor de la peau". Arch Gen Med (in French). 94: 693.
- Yu CC, Cook MG (June 1990). "Hidradenitis suppurativa: a disease of follicular epithelium, rather than apocrine glands". The British Journal of Dermatology. 122 (6): 763–9. doi:10.1111/j.1365-2133.1990.tb06264.x. PMID 2369556.
- Boer J, Weltevreden EF (November 1996). "Hidradenitis suppurativa or acne inversa. A clinicopathological study of early lesions". The British Journal of Dermatology. 135 (5): 721–5. doi:10.1111/j.1365-2133.1996.tb03880.x. PMID 8977671.
- Dessinioti C, Katsambas A, Antoniou C (May–June 2014). "Hidradenitis suppurrativa (acne inversa) as a systemic disease". Clinics in Dermatology. 32 (3): 397–408. doi:10.1016/j.clindermatol.2013.11.006. PMID 24767187.
External links
| Classification | |
|---|---|
| External resources |